Turn claims chaos into risk intelligence
Claims Discover ingests your full claims folder (reports, bordereaux, photos, notes) and extracts structured insights on root causes, loss drivers and emerging patterns that traditional systems miss.


Claims data shows what happened but rarely explains why
Root causes stay buried in expert reports, adjuster notes, legal correspondence and surveys. Without structured extraction, organisations can't systematically identify:
.svg)
Loss drivers and causal chains behind severity
.svg)
Wording intent vs. actual claim outcomes: disputes, exclusions, grey zones
.svg)
Silent drift in underwriting assumptions
Claims don’t fail in isolation. Risk emerges at portfolio level
Every claim carries signals about the wider portfolio. But traditional systems don't connect claim-level attributes to book-wide patterns:
.svg)
No automatic linking between claim factors and portfolio accumulation
.svg)
Underwriters forced to zoom in and out manually to build context
.svg)
Claims remain a cost when they should be your source of risk intelligence
From fragmented files to a single actionable risk picture
Claims Discover extracts, structures and centralises causal evidence from the claims record.
Every team works from the same standardised risk picture to identify patterns, challenge assumptions and trigger better decisions.

Underwriting
Feed claims-derived signals back into risk selection, pricing adequacy and referral triggers. Detect silent drift in assumptions before it reaches the loss ratio.

Portfolio management
Map severity drivers, peril combinations and accumulation patterns across the book. Move from reactive reserving to forward-looking exposure insight.

Policy wording
Surface ambiguity hotspots, coverage gaps and misalignment between wording intent and actual claim outcomes. Prioritise clause remediation where disputes and leakage concentrate.


End-to-end, from ingestion to decision
Claims Discover processes your full claims record end-to-end, so teams can focus on what matters: root causes, loss drivers and emerging patterns across the book.
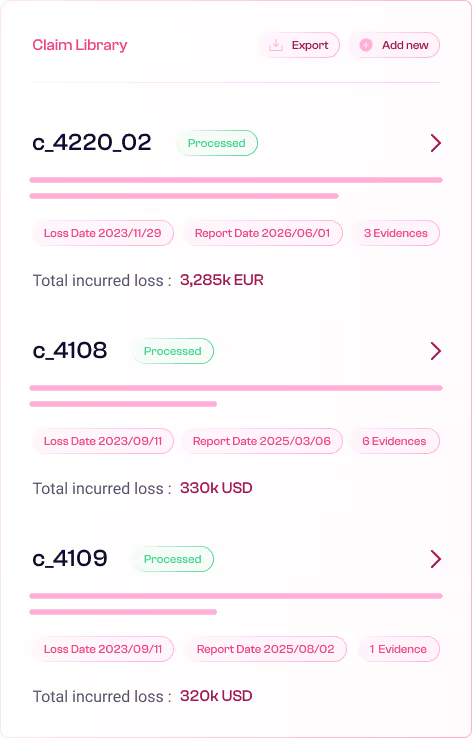







Extract causes. Detect patterns. Trigger decisions.
Claims Discover structures all claims information and delivers it as decision-ready signals. For every team, at every level of the portfolio.
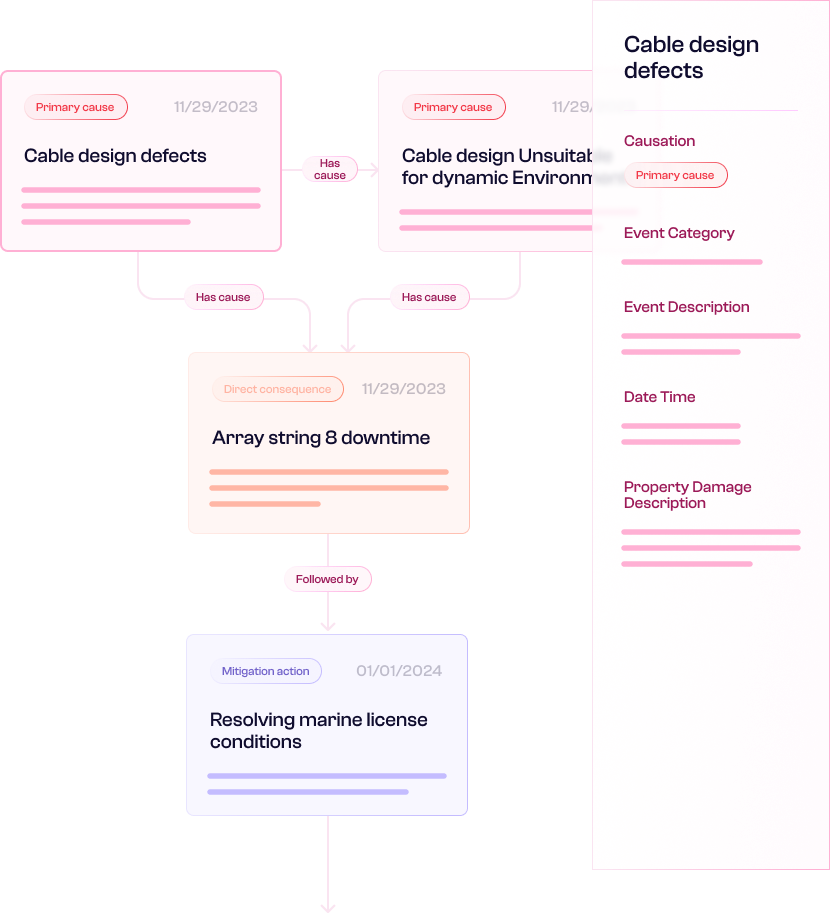
Knowledge extraction & causal grounding
Structure causation, liability, quantum and coverage data from the full claims file. Every insight traces to source evidence with hallucination reduced by design.

Referential normalisation & taxonomy management
Auto-build and govern normalised reference lists and risk classification frameworks. Aligned to your underwriting and exposure taxonomies.

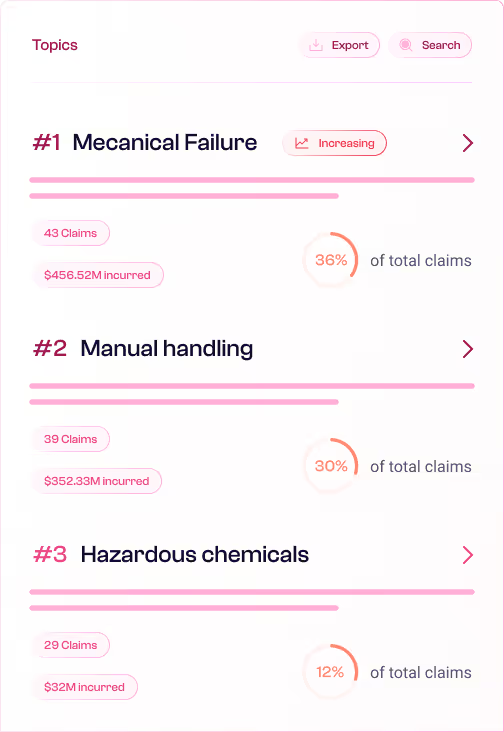
Pattern detection & severity analytics
Surface emerging loss patterns, contributing factor combinations and accumulation signals across lines, segments or programmes.

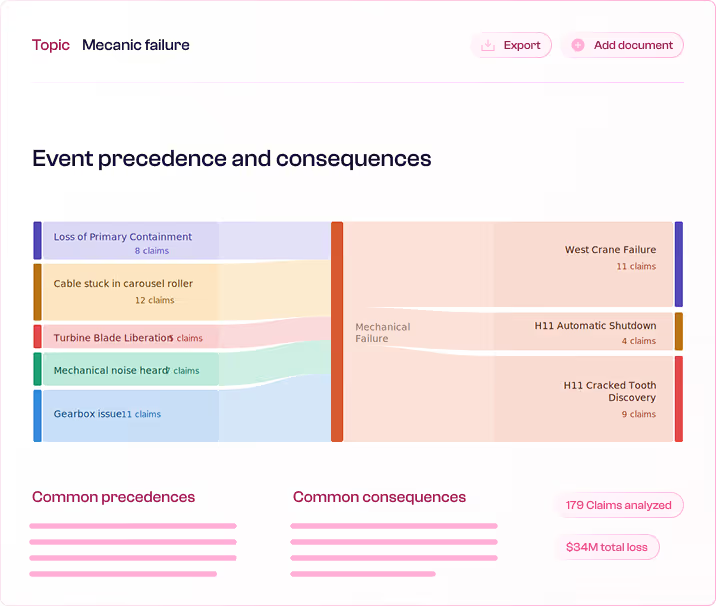
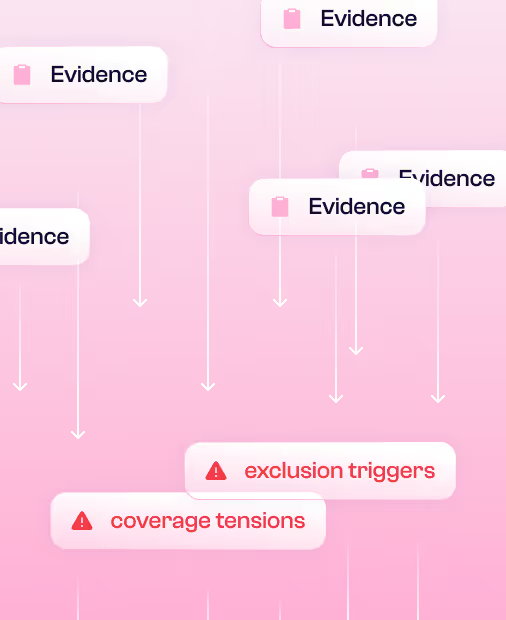
Flexible aggregation & wording observations
Slice by client, asset, location, peril or custom dimension. Flag coverage tensions and exclusion triggers with evidence, not anecdote.
Recommendations & risk learning loop
Generate decision-ready outputs: pricing signals, referral triggers, wording remediation, risk actions. Claims intelligence feeds back into the book continuously.

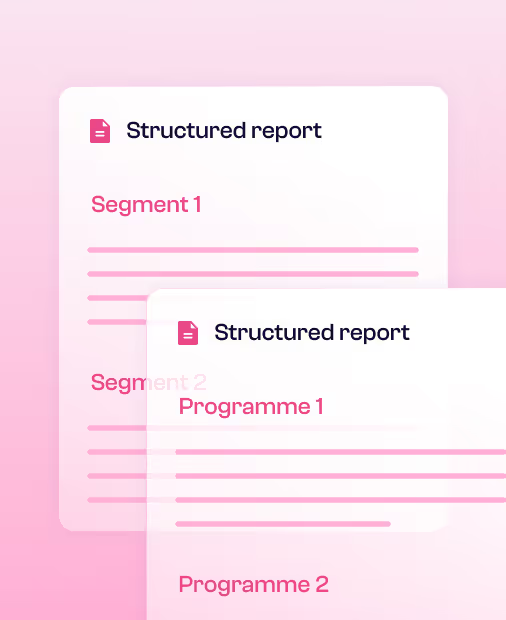
Portfolio reporting & client insights
Structured loss pattern reports by segment or programme. Share findings with insurance clients to support risk dialogue and retention.
Proven impact across many portfolios
When claims intelligence meets exposure data, underwriting and claims teams don't just understand the past, they reshape the book. Combined with exposure and premium data, these insights translate directly into tighter risk selection, more accurate pricing, targeted wording remediation and sharper reinsurance purchasing.
95% time saved
on manual claims coding and classification

120+ insight attributes
captured per claim on average, beyond what any traditional system codes

1,500 claims folders
ingested and structured in a single day

20 emerging patterns
identified per portfolio on average

4 risk intelligence recommendations
generated per emerging pattern on average

4× improvement
in claims data precision and consistency

20+ lines of business
analysed to date: casualty, property, specialty, life & health

Global reach
claims portfolios analysed across jurisdictions and regulatory environments

Why claims and portfolio teams choose Claims Discover
.svg)
Causal grounding
Manual coding, no causation chain
Probabilistic output, hallucination risk
DAG-based causal structure with confidence scoring
Cross-document extraction
Single document at a time
Limited context window
Stack across reports, notes, surveys, through time
Re-run & consistency
Full rework on change
Unpredictable variance
Re-run engine, revise criteria, maintain consistency
Multi-LOB workspaces
Rigid per-line config
No domain structure
Dedicated workspaces per line, programme or client
Knowledge graph backbone
Flat relational tables
No persistent structure
Graph database, agent-ready, cross-portfolio queries
Adaptability
Static reports
One-shot answers
Revise scope, escalation summaries, evolving taxonomies
Insurance-grade AI
Rule-based only
General-purpose model
Built for contracts, regulation and underwriting workflows
Expert templates
Build from scratch
Prompt engineering
Ready-to-use insurance configurations
Enterprise governance
Varies
Limited controls
Multi-region. GDPR, US standards,
How insurers put Claims Discover to work
Connects to your world. Doesn't replace it.
Claims Discover is not another claims system. It sits alongside your existing tools and makes them smarter.

API-first architecture
Ingest from any source, push insights to any downstream system.

Live in days, not weeks
Workspace configuration, taxonomy mapping and first results within a single sprint.

Your team, our support
Dedicated onboarding, domain experts who speak insurance, and continuous tuning as your questions evolve. We adapt to how your teams work, not the other way around.

Want to see Claims Discover in action?
Explore how your claims data can reveal portfolio insights. Schedule your custom demo



.svg)






.avif)
.avif)